|
Pathological diagnosis on the basis of immunohistochemistry and specific diagnosis methods such as radiological and serological assessments are important for providing rapid diagnosis and appropriate treatment. This patient underwent bilateral orchiectomy and adjuvant hormonal therapy and survived for 47 months after diagnosis of left supraclavicular node metastasis. Prostate-specific antigen levels and magnetic resonance imaging findings aided the diagnostic process. In the prostate carcinoma case, 18F‐fluorodeoxyglucose uptake was weak. He survived for 2 months after diagnosis of left supraclavicular lymph node metastasis. 
GATA3 staining aided in the diagnosis of urothelial bladder cancer with left supraclavicular node metastasis. Hematoxylin–eosin staining of the bladder lesion did not identify a clear glandular or squamous component, and we could not make a definitive diagnosis of whether the lesion was poorly differentiated squamous cell carcinoma, adenocarcinoma, or high-grade urothelial carcinoma. In the bladder carcinoma case, pathological analysis of fine-needle aspiration biopsy specimen of the metastatic cervical lymph node showed atypical cells with slight squamous differentiation. Palliative care only was given, with survival for 11 months after diagnosis of lymph node metastasis. In the cholangiocarcinoma case, carbohydrate antigen 19-9 and alpha-fetoprotein levels helped to diagnose cholangiocarcinoma. 
In these cases, adenocarcinoma was diagnosed based on left supraclavicular node biopsies, and a second primary tumor was found, in a 78-year-old Japanese woman with a diagnosis of cholangiocarcinoma, a 64-year-old Japanese man with a diagnosis of bladder carcinoma, and a 61-year-old Japanese man with a diagnosis of prostate carcinoma. We report three cases of malignant infradiaphragmatic tumor diagnosed following an initial finding of left supraclavicular node metastasis after surgery for tongue squamous cell carcinoma (follow-up period, range 18–62 months). When metastasis is detected in the left supraclavicular node in patients with head and neck carcinoma, locating the primary cancer remains a difficult and time-consuming challenge despite the dramatic development of screening technologies and treatment methods. It also always makes me a little bit nervous when my lymph nodes are swollen because I know that's symptom of lymphoma.Ī good friend of mine had a grandfather who passed away from lymphoma.Metastasis of infradiaphragmatic tumors to the left supraclavicular lymph node is reported to be rare. Swollen lymph nodes in the neck are just about the worst part of being sick. Swollen lymph nodes are a symptom of an infection and you may need an antibiotic! It is usually a good idea to go to the doctor anyway though. However if you have swollen lymph nodes along with symptoms of a cold you probably don't need to worry about cancer. June 22, - I can see why that would make you and your friend feel bit skittish about swollen lymph nodes. I have some other neuro problems, but no infection. I was worried about lymph node but the doctor felt it and said it was muscle disorder and there is no lymph node there. I have a swelling above my left collarbone below neck and towards the shoulder, slightly and rarely painful. What are the Most Common Causes of Lymph Node and Neck Pain?.What Are the Posterior Cervical Lymph Nodes?. 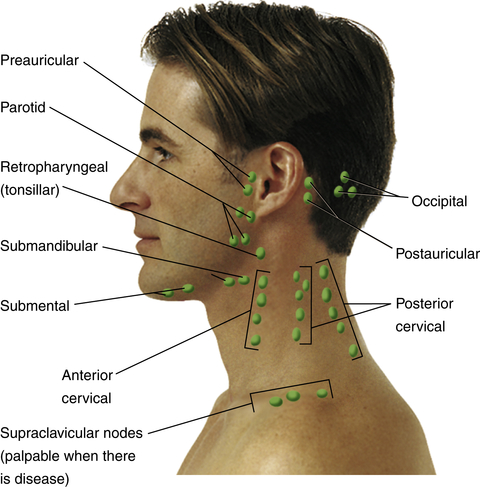
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
